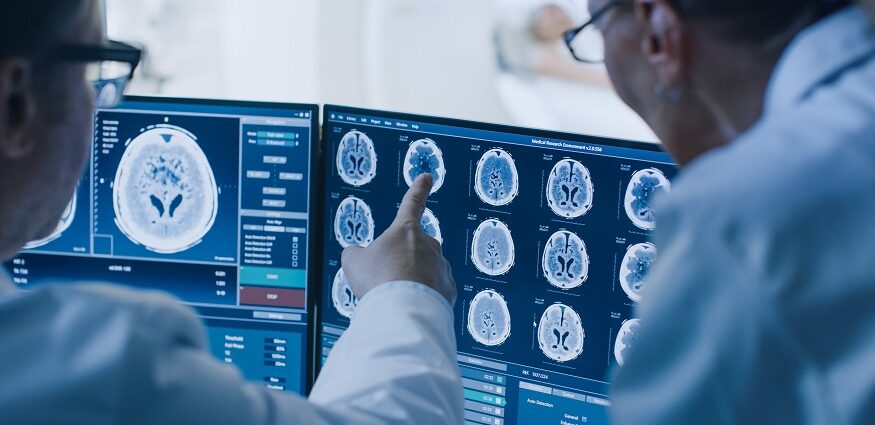
Diagnostic imaging refers to a variety of non-invasive techniques, such as x-rays, ultrasound, CT, MRI, and nuclear scans, that provide images of structures and activity inside the body. These images provide valuable information to assist doctors in making accurate diagnoses and planning appropriate treatments. Determining when to order quality diagnostic imaging requires balanced clinical reasoning. Overuse wastes healthcare resources and needlessly exposes patients to risks. Underuse delays or impedes proper medical care. This article explores guidelines physicians follow to determine appropriate uses for today’s quality diagnostic imaging.
Modern medicine relies extensively on quality diagnostic imaging throughout the continuum of care, from preventive screening in healthy individuals to disease staging in very ill hospitalized patients. Imaging capabilities to noninvasively peer inside human anatomy have grown tremendously in recent decades as technology modalities improve detection capacities through detailed digital imagery, precisely targeted scans, and innovative diagnostic analytics.
Quality diagnostic imaging requires tremendous resources and specialized expertise to safely acquire reliable images that appropriately answer a medical question. The highest standards are necessary to handle sensitive patient data and exposure to elements like radiation and strong magnetic fields during scans. Determining the correct usage is crucial for ethical patient care and public health. Misuse or overuse of tax-limited capacities while underuse negatively impacts care quality if treatable conditions go unidentified.
The following sections provide an overview of the evidence-based rationale physicians follow to determine appropriate quality diagnostic imaging deployment for optimal patient management while conserving resources.
Screening Asymptomatic Patients
In healthy individuals, quality diagnostic imaging plays an important role in early disease detection through scheduled general screening based on age, gender, or risk factors. Screening aims to identify certain conditions before symptoms arise, when potential treatments may be more effective or less invasive.
Widely adopted examples include mammography to screen for breast cancer starting at age 40, colon cancer screening starting at age 45, lung cancer screening for heavy former or current smokers starting at 50, abdominal aortic aneurysms screening for men ages 65-75 who smoked over 100 cigarettes in their lifetime, and osteoporosis screening for women over age 65. Quality organizations provide detailed screening protocol guidelines that physicians consult.
Evaluating New Patient Symptoms
A common reason for quality diagnostic imaging orders is to search for potential causes of symptoms appearing in new patients or unexplained symptoms in established patients. Examples include chest x-rays to evaluate respiratory symptoms like a stubborn cough or difficulty breathing, CT scans to assess severe abdominal pain, and brain MRIs to investigate neurological symptoms like debilitating headaches or extremity numbness. Quality diagnostic imaging aims to uncover anatomical abnormalities that may explain symptoms.
Monitoring existing conditions
Many conditions, once definitively diagnosed, warrant periodic quality diagnostic imaging surveillance to monitor disease progression and treatment efficacy. The frequency varies based on the diagnosis. For example, oncology patients may undergo CT, MRI, or PET scans every few months to check the effects of chemotherapy or radiation therapy on tumor size and metabolism. Rheumatoid arthritis patients may get annual MRIs to monitor inflammation progression in their hands and wrists. Quality imaging surveillance catches changes requiring medication or therapy adjustments for ideal disease management.
Guiding Interventional Care
Certain minimally invasive treatments utilize quality real-time diagnostic imaging to visually guide interventionists to targeted anatomy. Examples include CT-guided lung biopsies, ultrasound-guided breast biopsies, and fluoroscopy-guided steroid spine injections. Detailed visualization confirms needle trajectory to specimens and monitors injection dispersion patterns. Interventional procedures require the highest imaging quality to precisely operate interactive systems.
Emergency Settings
Emergency medicine relies extensively on rapid-quality diagnostic imaging for evaluating unstable patients with acute conditions that pose a disability or death risk if not treated urgently. Trauma teams use whole-body CT scans to catalog multi-system injuries. Emergency ultrasounds quickly identify blood pooling around vital organs that requires a rapid surgical response. Quality imaging is indispensable for expediting proper diagnosis and interventions for the best outcomes in emergency scenarios.
Justifying Requests
Quality medical practice includes documenting clear clinical rationale within patient medical records to justify requesting diagnostic procedures based on the patient’s history and symptoms. Appropriateness guidelines from reputable medical societies provide evidence-based criteria around how features of suspicion match with recommended imaging modalities for the highest yield at the lowest risk and cost. This decision framework aims to uphold quality standards that benefit individuals and public health.
Considering radiation exposure
Exposure to ionizing radiation through repeated CT scans or x-rays does carry small potential cancer risks down the road. However, quality imaging protocols always employ dose minimization principles, limiting scans to required areas and avoiding multiphase studies if not clinically indicated based on initial findings. Risks versus benefits must be weighed, but advances in low-dose CT make radiation less concerning for many scenarios.
Access and resource stewardship
As technology expands possibilities, costs also rise, impacting the accessibility of quality imaging. Responsible physicians consider expenses for patients and insurers when ordering scans, striving to conserve finite funding pools to best serve public interests. Appropriate, ethical standards for quality diagnostic medicine prevent misuse from inflating collective medical costs.
Research Applications
Quality imaging enables extensive research, advancing medical knowledge about anatomical structure and physiological function in healthy and diseased states. Studies utilize imaging to better understand disease pathways for developing treatments. Trials apply quality diagnostic imaging to accurately measure outcomes, assessing the safety and efficacy of interventions. Research propels top-quality diagnostic imaging technology innovation.
Artificial intelligence potentials
Quality imaging fields amass huge data sets well suited for artificial intelligence and deep learning applications. Algorithms can analyze images, identifying visual patterns imperceptible to humans that may indicate disease earlier. Augmented intelligence can also reduce repetitive tasks, improve workflow efficiencies, and minimize errors. AI promises to expand future quality diagnostic capacities and value.
Conclusion
The growth in capacity and capability of imaging technologies creates great potential to impact modern healthcare delivery across screening, diagnosis, treatment, and monitoring if leveraged appropriately as quality diagnostic tools. Determining the correct contexts for balancing risk, cost, access, and ethical use requires extensive medical training and responsible clinical reasoning grounded in scientific evidence. When deployed properly, today’s top quality diagnostic imaging affords invaluable visualization for improved detection, management, and recovery from prevalent health conditions.